Post Op Instructions
Extractions
There are times when it is necessary to remove a tooth. Sometimes a baby tooth has misshapen or long roots that prevent it from falling out as it should, and the tooth must be removed to make way for the permanent tooth to erupt.
At other times, a tooth may have so much decay that it puts the surrounding teeth and jaw at risk, so Dr. Cook may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
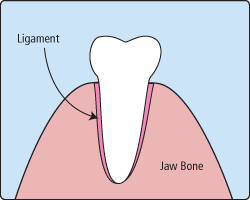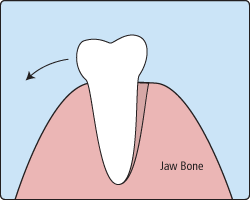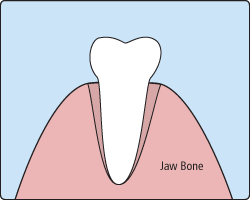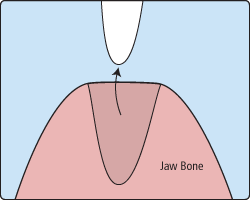
When it is determined that a tooth needs to be removed, a dentist may extract it during a regular checkup or schedule another visit for this procedure. The root of each tooth is encased within your jawbone in a “tooth socket,” and your tooth is held in that socket by a ligament.
In order to extract a tooth, Dr. Cook must expand the socket and separate the tooth from the ligament holding it in place. While this procedure is typically very quick, it is important to share with any of your concerns or preferences for sedation with our office.
Once a tooth has been removed, neighboring teeth may shift, causing problems with chewing or your jaw joint function. To avoid these complications, we may recommend you replace the extracted tooth.
Fillings
Traditional dental restoratives, or fillings, include gold, porcelain, and composite. The strength and durability of traditional dental materials make them useful for situations where restored teeth must withstand extreme forces that result from chewing, often in the back of the mouth.
Newer dental fillings include ceramic and plastic compounds that mimic the appearance of natural teeth. These compounds, often called composite resins, are usually used on the front teeth where a natural appearance is important, but they can also be used on the back teeth depending on the location and extent of the tooth decay.
What’s right for me?
Several factors influence the performance, durability, longevity, and expense of dental restorations, including:
- The components used in the filling material
- The amount of remaining tooth structure
- Where and how the filling is placed
- The chewing load the tooth will have to bear
- The length and number of visits needed to prepare and adjust the restored tooth
Before your treatment begins, Dr. Cook will discuss all of your options with you and help you choose the best filling for your particular case. In preparation for this discussion, it may be helpful to understand the two basic types of dental fillings: direct and indirect.
- Direct fillings are placed into a prepared cavity during a single visit. They include glass ionomers, resin ionomers, and composite (resin) fillings. The dentist prepares the tooth, places the filling, and adjusts it in one appointment.
- Indirect fillings generally require two or more visits. They include inlays, onlays, veneers, crowns, and bridges fabricated with gold, base metal alloys, ceramics, or composites. During the first visit, the dentist prepares the tooth and makes an impression of the area to be restored. He or she then places a temporary covering over the prepared tooth. The impression is sent to a dental laboratory, which creates the dental restoration. At the next appointment, the dentist cements the restoration into the prepared cavity and adjusts it as needed.
Dental Health and Root Canals
In the past, if you had a tooth with a diseased nerve, you would probably lose that tooth. Today, with a special dental procedure called root canal treatment, your tooth can be saved. Root canals are a relatively simple procedure involving one to three office visits. Best of all, having a root canal, when necessary, can save your tooth and your smile!
What is the purpose of a root canal?
A tooth’s nerve is not vitally important to its health and function after the tooth has emerged through the gums. Its only function is sensory: to convey the sensation of hot or cold. The presence or absence of a nerve will not affect the day-to-day functioning of the tooth.
When a tooth is cracked or has a deep cavity, bacteria can enter the pulp tissue and germs can cause an infection inside. If left untreated, an abscess may form. If the infected tissue is not removed, pain and swelling can result. This can not only injure your jawbones, but it is detrimental to your overall health. Without the proper treatment, your tooth may have to be removed.
What are the signs that a root canal is needed?
Teeth that require root canal therapy are not always painful. However, signs you may need a root canal include severe toothache, pain upon chewing or application of pressure, prolonged sensitivity or pain in response to hot and cold temperatures, a dark discoloration of the tooth, and swelling and tenderness in the nearby gums. If you experience any of these symptoms, contact our office.
What happens during a root canal?
Root canal treatment involves one to three visits. During treatment, a general dentist or endodontist (a dentist who specializes in problems with the nerves of the teeth) removes the affected tissue. Next, the interior of the tooth will be cleaned and sealed. Finally, the tooth is filled with a dental composite.
If your tooth had extensive decay, Dr. Cook may suggest placing a crown to strengthen and protect it from breakage. As long as you continue to care for your teeth and gums with regular brushing, flossing, and checkups, your restored tooth can last a lifetime.
Crowns
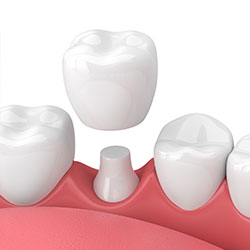
Crowns are a cosmetic restoration used to strengthen a tooth or improve its shape. Crowns are most often used for teeth that are broken, worn, or partially destroyed by tooth decay.
Crowns are “cemented” onto an existing tooth and fully cover the portion of your tooth above the gum line. In effect, the crown becomes your tooth’s new outer surface. Crowns can be made of porcelain, metal, or both. Porcelain crowns are most often preferred because they mimic the translucency of natural teeth and are very strong.
Crowns or onlays (partial crowns) are needed when there is insufficient tooth strength to hold a filling. Unlike fillings which apply the restorative material directly into your mouth, a crown is fabricated away from your mouth.
Your crown is created in a lab from your unique tooth impression, which allows a dental laboratory technician to examine all aspects of your bite and jaw movements. Your crown is then sculpted just for you so your bite and jaw movements function normally once the crown is placed.
Scaling & Root Planing
Scaling and root planing is one of the most effective, non-surgical ways to treat gum disease before it becomes severe. Scaling and root planing cleans between the gums and the teeth down to the roots.
Scaling is basically the process of removing dental tartar from the surfaces of the teeth. Root planing is the process of smoothing out the root surfaces and removing any infected tooth structure. If you have gum disease or gum pocketing, the gum pockets around the teeth will have deepened, thereby allowing tartar deposits to form under the gum line.
A careful cleaning of the root surfaces to remove plaque and calculus (tartar) from deep periodontal pockets and smoothing the tooth root to remove bacterial toxins will help ensure your gum disease is controlled.
Helpful Hints to Keep in Mind
- Scaling and root planing does not usually cause much discomfort, but you might experience some soreness afterwards, since deeper regions under the gums have been cleaned.
- Your teeth themselves may become a bit more sensitive to temperature, and bleeding might occur for a little while after your procedure.
- Over-the-counter painkillers such as ibuprofen work very well to alleviate discomfort, as do ice packs applied to the outside of the face around the treated area.
- Brushing and flossing will have to be done more gently to avoid aggravating any bruised or tender gum areas. We’ll show you the best methods for keeping your teeth clean during this time.
Scaling and root planing is a simple procedure that can work very well to stop gum disease. If you maintain good dental care after the procedure, the progression of your gum disease should stop, and your gums will heal and become firm and pink again in no time!


